Engineers developing COVID-19 tests for mass production, mass distribution
Posted Mar 24, 2021
Supported by more than $900,000 in federal grants, Iowa State University engineers are using their expertise in graphene-based biosensors to develop better, cheaper, quicker, more accessible testing for the coronavirus that causes COVID-19.
The studies are part of two federal programs looking for better ways to test for SARS-CoV-2, the virus that causes COVID-19 infections, and, potentially, any future viral outbreaks.
One study, supported by a one-year, $664,521 grant from the U.S. Department of Health and Human Services and the Centers for Disease Control and Prevention, is looking for effective tests that can be easily scaled up for mass manufacturing.
The other, supported by a two-year, $918,000 grant from the National Institutes of Health ($270,000 of which is designated for work at Iowa State) through the Rapid Acceleration of Diagnostics (RADx) program, is looking for tests that can be easily distributed to remote or vulnerable populations, such as employees of meat-processing plants.
“As soon as the pandemic started, we started thinking about using the sensor platforms we have developed to allow for easier testing and help with the pandemic,” said Carmen Gomes, an associate professor of mechanical engineering, a study leader and the chief research officer of NanoSpy, Inc., a biosensor startup based in the Iowa State University Research Park.
“We’re optimistic these sensors will work,” said Jonathan Claussen, also an associate professor of mechanical engineering, a project leader and chief scientific officer for NanoSpy. “The biggest challenge will be determining threshold levels for making a medical assessment of infection.”
The engineers’ project started with a $15,000 grant from Iowa State’s Office of the Vice President for Research to develop prototype COVID-19 tests. It has evolved into development of saliva tests similar to the test strips used to monitor glucose levels in people with diabetes. The tests look for the S1 spike protein of the coronavirus.
Claussen said tests could easily be done at home, workplaces or a doctor’s office, with no need for expensive laboratory instruments. Results will be displayed in about 20 minutes.
He expects total cost of the tests to be less than $6.
That buys a very sensitive test. Claussen said he expects it to detect viral concentrations down to trillionths of a mole. (Moles are a standard measure of 6.02214076 x 1023 particles within a substance, such as atoms or molecules).
A key to the technology is use of graphene, a supermaterial that’s a carbon honeycomb just an atom thick and known for its strength, electrical conductivity, flexibility and biocompatibility. Claussen and Gomes have used the material to print high-resolution electrodes for electrochemical sensors. They’ve developed the technology for a variety of applications, including making sensors to monitor food freshness and safety.
For the HHS/CDC project, Claussen said researchers will use aerosol jet printing technology to print prototypes of graphene electrodes for the sensors. The goal will be to find ways to convert the printing process to the gravure or screen techniques used in mass production.
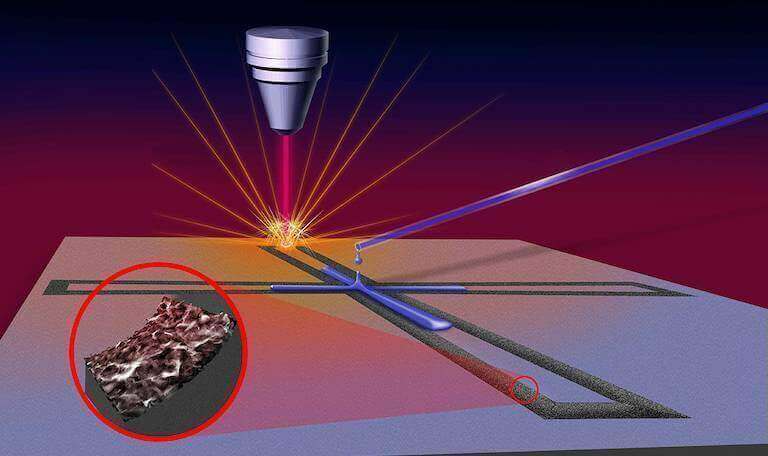
For the NIH project, Gomes said researchers are working on a one-step laser printing process to produce sensors. She said the NIH has been a valuable partner for the project, providing inactivated samples of the virus as well as saliva samples for testing.
She said the tests can be designed to detect variants of the virus using multiple sensing strategies for the same sample. And they’ll be designed to be long-lasting and work in all kinds of conditions – even a summertime testing center set up in a tent.
The engineers, after all, have used their graphene technology to develop soil sensors designed to be buried in the ground and keep working through hot, dry, wet or freezing soil conditions.
“I’m very excited about these projects,” Gomes said. “I do believe our platform can make tests low-cost, scalable and available to large segments of the population. People can easily do these tests.”
